Why Physicians Are Starting to Recommend Infrared Saunas — and Why Some Still Don't (2026)

Key Takeaways
- Infrared sauna moved from 'alternative medicine' to evidence-based medical journals in under a decade. Laukkanen in JAMA Internal Medicine (2015). Janssen in JAMA Psychiatry (2016). Mayo Clinic Proceedings review (2018). NIH-funded UCSF clinical trials (2024-2025). Sauna is now studied at the same level as pharmaceutical interventions
- Medical contexts where physicians currently recommend sauna: cardiac rehabilitation (Waon therapy in Japanese cardiology), chronic pain (integrative medicine), depression (UCSF protocol with CBT), rheumatology (fibromyalgia, RA), and sports medicine (post-exercise recovery). This isn't fringe — it's growing evidence-based integrative care
- If your doctor hasn't recommended sauna: medical school doesn't cover thermal therapy, the research base is young compared to pharmaceuticals, and it takes an average of 17 years for research to change clinical practice. The functional/integrative community adopted earlier. This isn't a criticism — it's how evidence adoption works
- When discussing with your physician: lead with specific studies (Laukkanen, Janssen, Mason), not wellness claims. Ask about medication interactions and contraindications. Physicians respect patients who bring evidence, not anecdotes
- The trajectory is clear: more research, higher-quality journals, larger institutions, growing acceptance. The question isn't whether sauna becomes standard complementary care — it's when
Ten years ago, if you told your cardiologist you were using an infrared sauna for heart health, you'd likely get a polite dismissal. Today, the evidence supporting that decision is published in the same journals your cardiologist reads — JAMA Internal Medicine, JAMA Psychiatry, Mayo Clinic Proceedings. The relationship between medicine and sauna has fundamentally changed.
The evidence trajectory: alternative to integrative
Before 2015: Sauna was 'alternative medicine.' Japanese Waon therapy research existed but wasn't widely known outside cardiology circles. Most physicians had no training in thermal therapy and no reason to recommend it. 2015: The Laukkanen cohort published in JAMA Internal Medicine — 2,315 men, 20+ year follow-up, 50% reduced cardiovascular mortality with frequent sauna. This put sauna into mainstream medical literature for the first time.
2016: Janssen et al. published in JAMA Psychiatry — an RCT showing single-session whole-body hyperthermia produced antidepressant effects lasting six weeks. Infrared heating technology. Depression is a condition every physician treats. 2018: Laukkanen and Kunutsor published a comprehensive review in Mayo Clinic Proceedings — sauna entered evidence-based medicine discourse at the highest level.
2024-2025: UCSF clinical trials using far-infrared sauna domes combined with CBT for major depression. NIH-funded. Active research at one of America's premier medical institutions. Multiple systematic reviews and meta-analyses published. Sauna is now being studied with the same rigor as pharmaceutical interventions.
Where physicians currently recommend sauna
Cardiac rehabilitation: Waon therapy is prescribed in Japanese cardiology for chronic heart failure — a meta-analysis of 491 patients showed improved ejection fraction and reduced BNP. Chronic pain management: Integrative medicine physicians recommend infrared sauna alongside physical therapy for fibromyalgia, arthritis, and chronic back pain.
Depression and mental health: UCSF's Ashley Mason studies infrared sauna as part of a depression treatment protocol combining heat with cognitive behavioral therapy — 86% of participants no longer met MDD criteria. Rheumatology: Oosterveld's study showed 40-60% pain reduction in inflammatory arthritis without disease exacerbation. Sports medicine: Post-exercise recovery protocols increasingly include sauna — the Ahokas 2025 study specifically validated infrared for athletic recovery.
The evidence physicians care about
Physicians don't respond to wellness marketing. They respond to study design, journal quality, and institutional credibility. The sauna evidence that moves medical minds: Prospective cohort with 20+ year follow-up (Laukkanen — gold standard observational evidence). Randomized controlled trials (Janssen 2016 — published in JAMA Psychiatry). NIH-funded clinical trials (Mason/UCSF). Systematic reviews (Hussain & Cohen 2018, Laukkanen & Kunutsor 2024). All published in journals physicians actually read.
Why your doctor might not know
If your physician hasn't mentioned sauna, it's not because the evidence doesn't exist — it's because of how medicine works. Medical school curricula don't cover thermal therapy. Most physicians have zero training in heat-based interventions. The research base, while growing rapidly, is still small compared to pharmaceutical evidence (which has thousands of trials per drug class). Many physicians are appropriately cautious about recommending anything without large, replicated RCTs.
It takes an average of 17 years for research findings to change clinical practice. The Laukkanen data is from 2015 — by that timeline, widespread physician adoption would come around 2032. The functional and integrative medicine community adopted earlier because they monitor emerging research more aggressively. This isn't a criticism of conventional medicine — it's how evidence adoption has always worked.
How to talk to your doctor about sauna
Don't say: 'I read online that saunas cure [condition].' Do say: 'I've been reading about passive heat therapy and the Laukkanen cardiovascular data published in JAMA Internal Medicine. I'd like to add regular sauna use to my wellness routine — are there any contraindications given my medical history and medications?'
Bring a printed summary of 2-3 relevant studies specific to your condition. Ask specifically: 'Are any of my medications affected by heat exposure or dehydration?' Physicians respect patients who bring evidence, not anecdotes. Framing sauna as a complement to your existing treatment — not a replacement — makes the conversation productive.
Notable researchers in the field
Jari Laukkanen (University of Eastern Finland): The Kuopio Ischaemic Heart Disease study. 20+ years of prospective data on sauna and cardiovascular/cognitive outcomes. The most-cited researcher in sauna medicine. Ashley Mason (UCSF): Clinical psychologist running NIH-funded trials on infrared sauna + CBT for depression. Chuwa Tei (Kagoshima University): Inventor of Waon therapy for chronic heart failure. Rhonda Patrick (FoundMyFitness): PhD researcher who popularized the dynorphin/endorphin framework and sauna science for the public.
Frequently asked questions
Frequently Asked Questions
Increasingly, yes — particularly in integrative medicine, cardiology (Waon therapy), pain management, mental health (UCSF depression trials), and sports medicine. Conventional medicine is slower to adopt, which is normal — research-to-practice takes an average of 17 years. The evidence is published in the same journals physicians trust (JAMA, Mayo Clinic Proceedings), and adoption is accelerating.
Yes — especially if you take medications. Some drugs interact with heat exposure (beta-blockers, diuretics, lithium, transdermal patches). Your doctor should know about any wellness practices that affect your physiology. Frame it as information-sharing, not asking permission. See our medication interactions guide for specific drug considerations to discuss.
Medical education doesn't cover thermal therapy. The research, while strong, is still young compared to pharmaceutical evidence. And physicians are trained to be conservative with recommendations — they wait for large, replicated RCTs. This is appropriate caution, not ignorance. The integrative medicine community adopted earlier because they actively seek emerging evidence for non-pharmaceutical interventions.
For cardiovascular: Laukkanen et al. 2015 (JAMA Internal Medicine). For depression: Janssen et al. 2016 (JAMA Psychiatry). For a comprehensive overview: Laukkanen & Kunutsor 2024 (Temperature journal). For heart failure specifically: the Waon therapy meta-analysis (Källström 2018). These are published in journals physicians recognize and trust.
It's in transition. The evidence base is substantial and growing — published in top-tier journals, studied at major institutions, funded by NIH. It meets the threshold for 'evidence-based complementary therapy' in many medical frameworks. It doesn't yet have the depth of evidence that pharmaceutical interventions do (thousands of RCTs). The trajectory is clearly toward greater acceptance.
Yes — unstable angina, recent heart attack, severe aortic stenosis, decompensated heart failure, active fever, and certain medication interactions are contraindications. See our heart health page for cardiac specifics and our medication interactions guide for drug-specific concerns. Always discuss with your physician if you have a serious medical condition.

Founder & Lead Designer, SaunaCloud®
3,000+ custom saunas built since 2014 · Author of The Definitive Guide to Infrared Saunas · Featured in Forbes, Inc., and MSN
Chris has been designing and building custom infrared saunas since 2014. He wrote one of the first comprehensive books on infrared sauna therapy and is personally involved in every SaunaCloud build — from design consultation through delivery and beyond.
Continue Reading
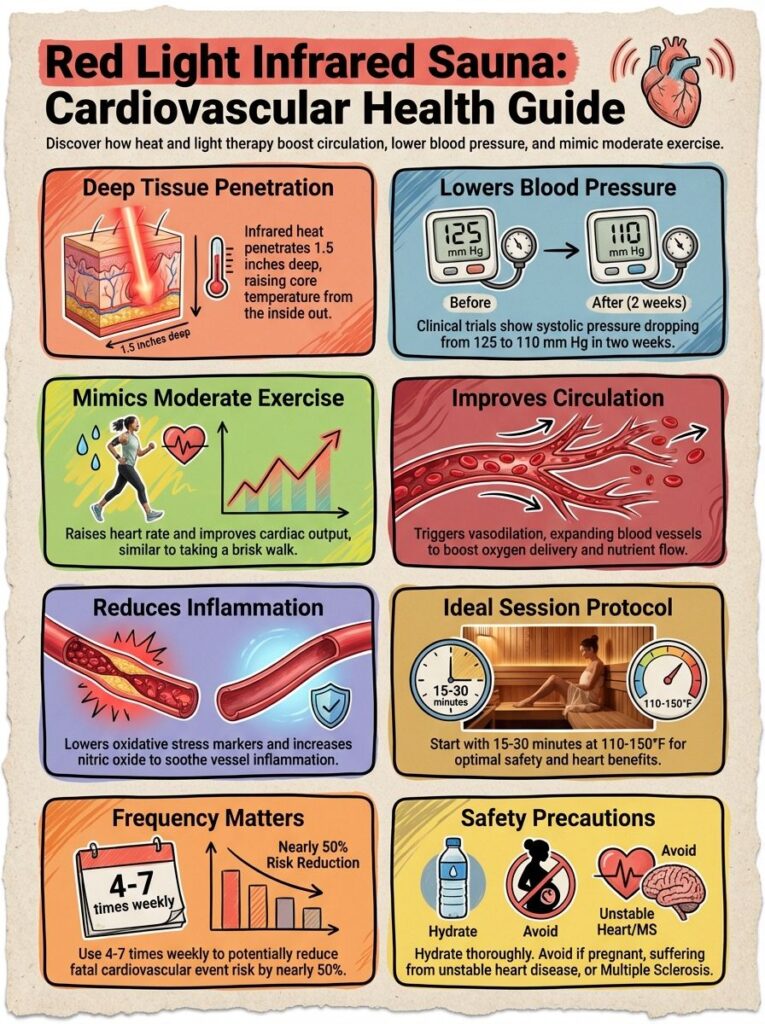
Infrared Sauna and Heart Health: From Prevention to Treatment — What the Cardiology Research Shows (2026)
Read article
Infrared Saunas and Blood Pressure: The Observational Promise and the RCT Reality (2026)
Read article
Getting High Naturally: The Complete Neurochemistry of the Infrared Sauna Euphoria (2026)
Read articleBuild the Sauna Your Integrative Physician Would Recommend
VantaWave heaters operating in the same wavelength range used in clinical research. Designed to the standard the evidence demands. Call 800-370-0820.